Error 556570 Has Occurred Pleas Wait a Little While and Try Again
Introduction
Critically ill patients with severe diseases and multisystem organ failure are currently frequently admitted to and treated in the intensive care unit (ICU). Although the identification and management of multisystem organ failure has improved, the incidence has increased over the last half-century1. Therapeutic options in the setting of multisystem organ failure are mostly aimed at supporting vital functions. The kidneys are almost e'er involved in such a syndrome, and dialytic techniques are routinely used in the ICUs to treat severe acute kidney injury (AKI)2.
Electric current do in renal replacement therapy (RRT) for adult critically ill patients, with specific details on technical features and clinical applications, volition be reviewed.
Technical problems
The technological evolution of RRT
Peter Kramer in 1977 described the starting time continuous form of dialysis specifically defended to critically ill patients: continuous arterio-venous hemofiltration (CAVH)iii. In CAVH, claret menstruation in the circuit was driven by a spontaneous arterio-venous pressure gradient and spontaneous ultrafiltration (UF) occurred depending on the transmembrane pressure level (TMP) slope. The arterio-venous force per unit area gradient was dependent on the mean arterial pressure of the patient and the intrinsic resistance of the excursion (determining the blood flow); the UF was determined by the hydrostatic pressure drop inside the filter and the negative suction provided past the UF column from the patient level to the ground. Equally a consequence, patients with low blood pressure and/or low cardiac output achieved the everyman clearances simply were able to self-limit UF. When peristaltic pumps were added to the extracorporeal circuit, veno-venous hemofiltration became viable. Subsequently, fluid delivery systems and UF control mechanisms were implemented assuasive dialysate and replacement solutions to be delivered with acceptable accurateness. Higher clearances were finally possible considering of the power to provide increased flow rates. Although conspicuously improved, RRT machines were still inaccurate, and rubber and functioning were still a challenge. Information technology shortly became axiomatic that an ideal extracorporeal excursion requires continuous pressure level measurements at different levels (inlet and outlet of vascular access, inlet and outlet of the filter and UF ports)4.
Currently, third/fourth-generation machines are designed to meet the dialysis dose requirements and the strict safety features that are recommended in every modern ICU5. Contemporary devices, equipped with 4 to 5 roller pumps, three to 4 scales and pressure sensors, permit a fluid load from twenty to 40 kg in guild to reduce nursing workload. In addition, maximal menstruum rates take increased up to about 450 mL⁄min for the blood pump, 8–10 50⁄hr for the dialysate⁄replacement pumps, and twenty–25 L⁄60 minutes for the effluent pump. Mechanical implementation has been associated with a huge electronic evolution: interfaces have been implemented with wide screens and clear alarm signals and warnings, and circuit force per unit area trends are at present visualized. Furthermore, during continuous RRT (CRRT), now flexible and prophylactic, modalities can be switched in order to tailor them to the patients' demand. Modern RRT filters, a central component of the system, are composed of groups of hollow fibers with a range of surface areas (from 0.ane to over 2 m2) in society to meet the need of differently sized patients. Such fibers have a generally high porosity (thirty–50 A°) with a pore cutoff size of 30 kDa and are used for both diffusive and convective treatments. Polyacrylonitrile, polysulphone and poly(methyl methacrylate) (PMMA) are the near unremarkably used membranes and allow a high UF coefficient (over 20 ml/h/mmHg) and high diffusive and convective performance. Biocompatibility (the change in blood factors induced by membrane/claret contact) is considered the nigh important quality of these RRT membranes.
Diffusion and convection
Renal replacement consists of blood purification by semi-permeable membranes. Blood flows into hollow fibers composed of porous biocompatible synthetic material. A wide range of substances (h2o, urea, depression, center and high molecular weight solutes) can be transported beyond such membranes, from the claret to the effluent side of the hollow fibers, by the mechanism of improvidence (solutes) and convection (water and solutes) (Figure 1).
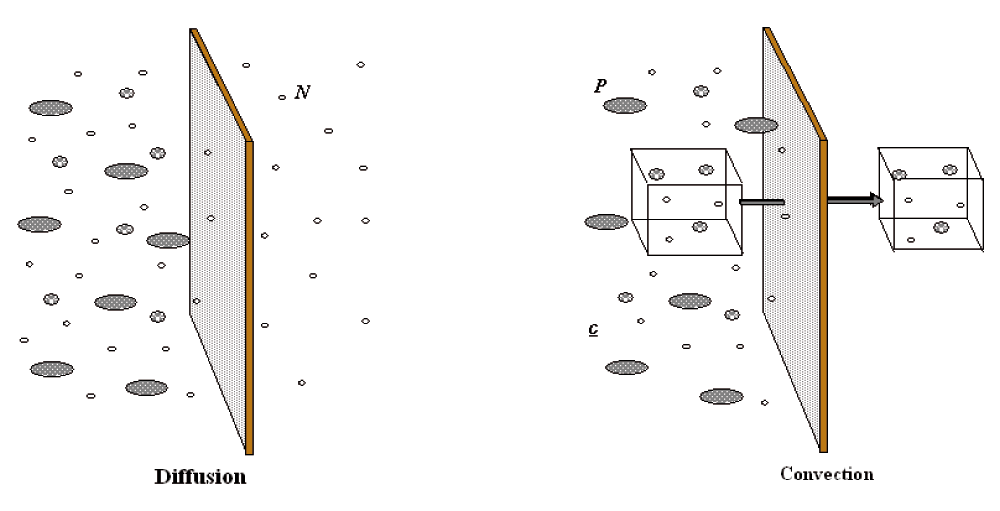
Figure one. Diffusion and convection are schematically represented.
During diffusion solutes flux (Jx) is a function of: solutes concentration gradient (dc) betwixt the two sides of the semi-permeable membrane, temperature (T), diffusivity coefficient (D), membrane thickness (dx) and surface expanse (A) according to the following equation: Jx = D T A (dc/dx)
Convective flux of solutes (Jf) requires instead a pressure gradient between the ii sides of the membrane (transmembrane pressure TMP), that moves a fluid (plasma water) with its « crystalloid » content (a process called ultrafiltration, whose entity is besides dependent on membrane permeability coefficient (Kf). Colloids and cells will not cross the semipermeable membrane, depending on the pores' size. Jf = Kf × TMP
Dialysis is based on the diffusion principle: a dialytic solution flows through the filter counter current to blood flow in order to maintain the highest solute gradient from inlet to outlet port. Diffusion is the solute ship method practical during intermittent hemodialysis (IHD) and continuous veno-venous hemodialysis (CVVHD) (Figure 2). During diffusion, the movement of solutes depends on their trend to achieve the same concentration on each side of the membrane, allowing the passage of solutes from the compartment with the highest concentration to the compartment with the lowest concentration. Other components of the semi-permeable membrane that affect diffusion include thickness and surface area, dialysate temperature, and diffusion coefficient.
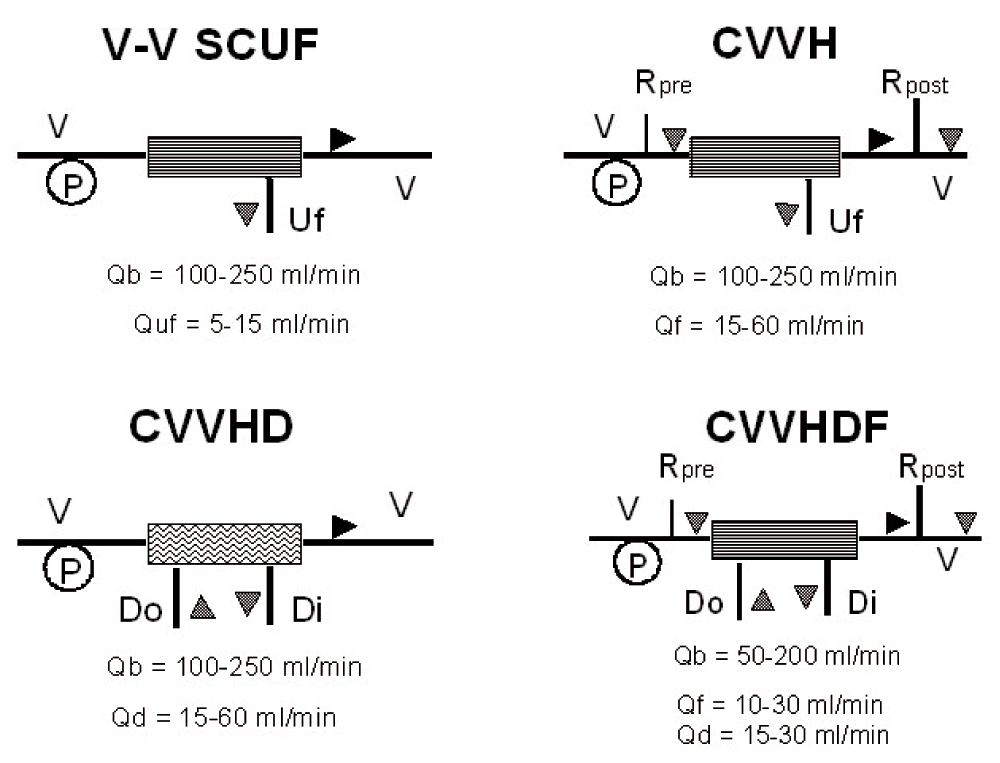
Figure 2. Schematic representation of most common continuous RRT prepare-ups.
Black triangle represents claret flow direction; gray triangle indicates dialysate/replacement solutions flows. V-5: veno-venous; Uf: ultrafiltration; Rpre: replacement solution prefilter; Rpost: replacement solution postfilter; Practise: dialysate out; Di: dialysate in; Qb: blood flow; Quf: ultrafiltration flow; Qf: replacement solution flow; Qd: dialysate solution flow.
During convection, solutes are transported beyond a semi-permeable membrane by UF (h2o transfer across the membrane). In other words, as the solvent (plasma water) is pushed (ultrafiltered) across the membrane according to the TMP, solutes are carried with it, as long as the porosity of the membrane allows the molecules to exist sieved from the blood. Convection is practical during continuous veno-venous hemofiltration (CVVH) while the combination of both convection and diffusion configures continuous veno-venous hemodiafiltration (CVVHDF) (Effigy ii).
The UF rate (QUF) in CAVH systems was governed past the membrane UF coefficient (Km) and the TMP slope generated by the pressures on both sides of the hollow fiber according to the post-obit formula:
QUF = Km * TMP
In modern RRT machines QUF is regulated by a pump and, consequently, it is constantly maintained regardless of whether the filter is "fresh" (when UF occurs with depression TMP) or clogging (in which case a progressive secondary increase of TMP is observed). In fact, as molecules cleared during convection are physically dragged to the UF side, the protein layering that progressively clogs the fiber pores significantly limits solute ship6. A peculiar membrane capacity, defined every bit adsorption, has been shown to play a major role in higher molecular weight toxinsvii; all the same, membrane adsorptive capacity is generally saturated within the first few treatment hours. This observation explains the minimal impact of the adsorption component on solute clearance8. An exception on this rule is made past high-mobility group box i poly peptide (HMGB-1), every bit this major sepsis cardinal mediator can be significantly removed (more than 90%) by adsorption through an acrylonitrile-treated surface (AN69-ST) and PMMA membranes9. However the clinical relevance of this molecule clearance remains to exist ascertained. Equally UF proceeds and plasma h2o and solutes are filtered from blood, hydrostatic force per unit area within the filter declines and the event of oncotic pressure increases because blood concentrates and hematocrit increases. The fraction of plasma h2o that is removed from claret during UF is called the filtration fraction and should be kept in the range of twenty–25% in guild to avoid equalization of the oncotic pressure to the TMP and filtration/pressure level equilibrium. Finally, replacing the plasma water removed through the filter with a exchange solution completes the hemofiltration process and purified blood is returned to the patient. When the commutation fluid is administered after the filter it is referred to as postal service-dilution HF. When the substitution solution is infused before the filter it is referred to as pre-dilution HF. While post-dilution allows a urea clearance equivalent to therapy delivery (meet below), pre-dilution, in spite of theoretical reduced solutes clearances, allows prolonged circuit lifespan by reducing hemoconcentration and protein caking furnishings within filter fibers. The difference between the volume of ultrafiltered plasma water and reinfused substitution solution gives the internet UF, which is the fluid that is eventually removed from the patient for fluid control. Net UF prescription is based on patient needs and can range from more than than one L/h (pulmonary edema in a patient with congestive middle failure and diuretic-resistant AKI) to zero (sepsis with catabolic country increased creatinine levels and conserved diuresis). A net UF rate must be added to improvidence-based CRRT modalities in club to attain fluid residue control since diffusion does non allow for water exchanges.
Interestingly, apart from the demonstration of different clearances of heart molecular weight solutes (i.e beta-2 microglobulin) provided by CVVH when compared to similar CVVHD dosesviii, no written report so far has shown that the application of hemofiltration, with respect to hemodialysis, improves hard outcomes (such every bit mortality, length of mechanical ventilation, length of hospital stay)x,11.
RRT dose
RRT dose is a mensurate of the quantity of blood purified past "waste material products and toxins" and is more often than not expressed every bit clearance (1000). Clearance is divers as the amount of claret purified past a unmarried solute in the unit of time and it is expressed as volume over fourth dimension, as it represents the flow of "cleaned" blood. As these notwithstanding incompletely known substances "to exist purified" are hard to measure and quantify, the operative view of RRT dose is mostly reduced to the measure out of the elimination of a representative marking solute. Unfortunately, the mark solute does not represent all the solutes that accrue during AKI because kinetics and volume of distribution are different for each solute and its removal during RRT is not necessarily representative of the removal of other solutes. However, since single solute marker assessment of dialysis dose appears to be related to patient outcome12, urea and creatinine, due to their pregnant accumulation during AKI and the ease of their routine daily blood decision, are generally used as reference solutes for measuring renal replacement clearance during either chronic or acute dialysis.
During RRT, clearance depends upon blood catamenia rate (Qb), substitution period rate (Qf) or dialysis flow (Qd), solute molecular weights, and hemodialyzer blazon and size. Qb is mainly dependent upon vascular admission and the operational characteristics of utilized machines in the clinical setting. Qf is strictly linked to Qb, during convective techniques, by filtration fraction. Filtration fraction does not limit Qd, just when Qd/Qb ratio exceeds 0.3, dialysate will not be completely saturated with blood diffusing solutes. When UF is applied, molecules are dragged with plasma h2o through the filter pores according to their sieving coefficient (SC); the SC is calculated as the effluent/plasma concentration ratio of the target molecule. When the SC is 1, as in the case of small molecules (below 12 kD, such as creatinine and urea), the same solute concentration is found in the two sides of the hollow cobweb. A SC value of 0 means that the molecule is non filtered (i.e. albumin, hemoglobin, etc). G during convection is measured by the product of Qf multiplied past the SC; hence, there is a linear relationship between Yard and Qf, the SC being the irresolute variable for different solutes. During diffusion, the linear human relationship is lost when Qd exceeds about i/3 of Qb.
I of the crucial claim of specific dose prescription, calculation, and delivery is the avoidance of underdialysis and the improved monitoring and awareness of effective delivered therapy.
Continuous vs intermittent RRT
Blood purification tin exist accomplished in the ICU both by continuous and intermittent RRT. In theory, during continuous RRT, the treatment is kept running 24 hours a day, vii days a week. During intermittent RRT renal support is delivered in intermittent sessions lasting (depending on centre preferences, protocols, and the patient's clinical condition) 3–vi hours, typically three times per week (or depending on specific needs). Currently, near 80% of critically ill patients are treated with continuous RRT. Still, due to the absence of significant differences in event deriving from the application of continuous vs intermittent RRT, no specific recommendation is provided past the major critical intendance societies, and the pick is mainly left to institutional protocols and expertise. Apart from bear witness in big clinical trials, more gentle RRT application is mostly improve tolerated in hemodynamically unstable, critically ill patients with astringent AKI. Furthermore, since the occurrence of intradialytic hypotension is proportional to the internet Quf charge per unit, it is possible to prescribe a lower internet Quf rate when the treatment is applied over 24 hours as compared to a quick 3-hour session. Recently, the Surviving Sepsis Campaign guidelines for management of severe sepsis and septic shockxiii concluded that, based on present scientific evidence, continuous RRT should be considered equivalent to IHD for treatment of AKI. Vinsonneau and colleagues14 conducted a large, prospective, randomized multicenter study in 21 ICUs over a 3.v-year period. The primary end bespeak was the threescore-day mortality following the randomization of 360 patients with AKI to either CVVHDF or IHD and no difference was found in 28, 60 and 90-mean solar day mortality between the ii groups. Hence, co-ordinate to the results, the study investigators ended that IHD can exist delivered safely to critically ill patients. Unfortunately, delivered dose in both artillery was non controlled for in the trial design. The accompanying editorialfifteen emphasized that the advantages of continuous therapies are particularly significant when therapy reanimation is minimized, in order to heighten the low intensity, shine and continuous effects of plasma G. However, Vinsonneau et al.'s findings have been confirmed repeatedly by other studies16,17. One of the reasons for the lack of hard outcome differences between intermittent and continuous techniques could be because IHD has go safer and more efficaciouseighteen. Alternatively, a liberal awarding of CRRT (including extended and probably incorrect indications) can cause adverse effects as discussed later beneath.
Hybrid techniques, which combine the advantages of both continuous and intermittent modalities, may represent an interesting compromise. Although a multifariousness of names have been given to hybrid techniques (meet the nomenclature section)19–22 depending on variations in schedule and type of solute removal (convective or diffusive), they all attempt to provide a gentle, prolonged and more feasible extended IHD, with all the advantages of discontinuous handling (less need for anticoagulation, increased patient mobility, easier possibility of plumbing equipment prescribed schedules without downtime). These techniques generally take shown practiced results in terms of hemodynamic tolerance and adequacy of dialytic dosage23. Baldwin and coworkers compared 3 consecutive days of CVVH with a similar flow of extended daily dialysis with filtration23. No significant difference was institute between the two therapies as far as urea or creatinine levels and electrolyte and acid–base of operations control. Interestingly, after 3 days of treatment, there was a mild but persistent metabolic acidosis in the extended dialysis group, but in the CVVH group hypophosphatemia was described. Advantages and disadvantages of IHD, CRRT and hybrid techniques, respectively, are depicted in Table 1.
Tabular array 1. Intermittent vs Continuous vs Extended Dialysis.
| Advantages | Disadvantages | Contraindications | |
|---|---|---|---|
| Intermittent Hemodialysis (IHD) | • Short elapsing • No/short/less anticoagulation (reduced risk of bleeding). • Higher efficiency for immediate small water-soluble removal (life-threatening hyperkalemia) • Less bed rest • Flexibility of apply: machines tin exist used in an extended protracted mode (increase in efficacy) • Bags cost saving | • Technical skills (trained personnel) and technical infrastructure (dedicated areas with h2o connection) • Clearance rebound • Hemodynamic touch/instability • Potential college risk of dialysis dependence | • Traumatic brain injury |
| Continuous Renal Replacement Therapy (CRRT) | • Hemodynamic stability (less cardiovascular impact) → college potential recovery of kidney function • ICU staff may handle these treatments apart • Superior solute removal and volume control (in a 24 hours lasting session) • Assistants of parenteral nutrition fluids | • Reanimation may impair efficiency • Continuous systemic (heparin) or regional (citrate) anticoagulation (higher risk of patient'due south bleeding or filter clotting) • Bed rest is necessary • Higher cost • Lower efficiency than IHD (hyperkalemia) • Take chances of hypothermia | • Patients needing mobilization |
| Sustained Low-Efficiency Daily Dialysis (SLEDD) or Prolonged intermittent RRT (PIRRT) | • Piece of cake • Expert flexibility of sessions administration (half dozen–12 hours or overnight treatment) • College possibility for patient mobility • Hemodynamic stability • Relatively low anticoagulation requirement • Bags price saving | • Technical skills (trained personnel) and technical infrastructure (dedicated areas with water connection) • Hypophosphatemia • Hypothermia • Low efficiency | • None |
In conclusion, intermittent and continuous therapies, when applied by proficient centers, may appear similar where hard outcomes are concerned. As far every bit long-term RRT outcomes are concerned, however, recent reports bespeak that RRT survivors treated by IHD might take a lower run a risk of recovering pre-morbid kidney function and have an increased risk of remaining dialysis-dependent at hospital discharge24.
Anticoagulation
The contact between blood and bogus surfaces induces activation of the coagulation cascade, resulting in filter and/or excursion clotting and the need for anticoagulation25–29. Anticoagulation strategy depends on the blazon of RRT and is often needed for continuous therapies due to the increased exposure to the blood-artificial surface. Aims of anticoagulation are: maintenance of extracorporeal excursion and dialyzer patency; reduction of reanimation that might have a clinical touch on in the overall RRT clearance; reduction of treatment price by the utilization of less material; and achievement of the above aims while minimizing risks for the patient. Several technical features of the RRT excursion are likely to touch on the success of any anticoagulant approach: vascular access has to be of acceptable size; tube kinking should be avoided; blood menstruation rate should exceed 100 ml/min; pump flow fluctuations must exist prevented; and the venous bubble trap, where air/blood contact occurs, must be accurately monitored. Furthermore, plasma filtration fraction should exist kept equally far as possible below xx% and, when possible, pre-dilution hemofiltration should be selected. There is evidence that, when circuit fix-up is perfectly optimized, anticoagulants are simply a relatively minor component of circuit patency. When patients have altered coagulation, thrombocytopenia, or active bleeding (e.g. after trauma or surgery), RRT can exist safely performed without anticoagulation25. Lastly, regional citrate anticoagulation (RCA) tin exist safely used nowadays not simply in patients with bleeding risks merely too in patients without haemorrhage risks, according to the electric current KDIGO guidelines30. Extensive preparation is needed regarding the metabolic side effects of citrate before embarking upon routine citrate anticoagulation. In recent years, new commercially available citrate solutions together with adapted CRRT machines have rendered the technique safer and easier to use31.
Different methods for anticoagulation are summarized in Table 2.
Table 2. Anticoagulation strategies.
| Drug | Indication | Contra | Comment |
|---|---|---|---|
| No anticoagulation | Loftier risk bleeding profile | Relative shorter excursion lifespan | RRT tin be safely performed without anticoagulant |
| UFH | Routine | Striking | Antidote is available (protamine). Monitoring: aPTT. Serum antithrombin levels accept to be optimized |
| LMWH | Routine (alternative to UH) | HIT | Ameliorate bioavailability than UFH |
| PGI2 | Very curt circuit lifespan | Hypotension | Strong inhibitor of platelet aggregation with a short half- life. Hypotension might occur. Its loftier cost and harmful side effects might limit the utilize |
| Citrate | Routine/Very brusk circuit lifespan | Hypocalcemia | Regional anticoagulation. Calcium is chelated in the filter and then calcium chloride is infused dorsum to the patient to maintain normocalcemia. Excellent filter patency. Relative drawbacks include the risk for hypocalcemia, metabolic alkalosis/acidosis, and the cumbersome replacement/dialysate fluid training |
| Danaparoid | Striking | Insufficient data bachelor | |
| Argatroban | HIT | Insufficient information available | |
| Irudine | HIT | Insufficient data available | |
| Nafamostat mesilate | HIT | Insufficient data available | |
| Heparin coated circuits | Routine | Insufficient data available |
Clinical applications
Indications to start RRT
Regardless of RRT technique used, the post-obit clinical variables are typically compromised in the critically ill patient with AKI: fluid condition and tissue edema, hemodynamics, acid–base and electrolyte equilibrium, protein-rich nutritional support, phosphate and calcium balance, and infection control.
Currently, a broader concept of "timely intervention" is generally accepted. When oliguria results in impairment of one or more of the to a higher place clinical variables, RRT should be instituted rapidly in club to avoid fluid overload and congestion. The simply urgent indications to perform dialysis are pulmonary edema refractory to high dose diuretics, rapidly increasing hyperkalemia, severe refractory acidosis, symptoms/signs of uremia, and specific drug intoxications. Critically ill patients, particularly if they are oliguric or anuric, typically gain weight from water accumulation and large volumes of intravenous fluids. In such patients, water removal is indicated for the achievement of a negative daily fluid remainder, which has been associated with multiorgan function comeback (i.e. at the pulmonary, cardiac and renal level) in observational and retrospective studies32,33. Furthermore, a slow continuous RRT with fluid removal over 24 hours is better able to manage the critically ill patient's needs; in case of increased nutritional administration, fluids deriving from parenteral drugs or hemoderivates transfusion, QUF can be easily tailored on an hourly base34. Conversely, rapid (or, worse, intermittent) ultrafiltration of body h2o may pb to acute hypovolemia and subsequent hypotension, since refilling from the interstitial compartment is slow and steady due to hydrostatic and osmotic pressures35. Since no effective clinical monitoring is currently available to "measure out" fluid overload and the amount of fluid excess to be removed, clinical expertise in critical intendance nephrology (and possibly a multidisciplinary arroyo) is essential for acceptable management of fluid removal36.
As for the verbal timing for starting RRT, a definition of timing is currently not bachelor. Timing tin can be considered as a synonym for "indication" and and then 1 can start CRRT early or belatedly depending on how severe (or conventional) the indication is (e.g. creatinine level or potassium level or the presence of sepsis)37. Otherwise, timing can be considered as the time elapsed between any established indication to start and the constructive inception of the dialytic session. A recent retrospective study38 confirmed that crude 90-twenty-four hours mortality of patients with RRT started later on "classic indications" (identified as hyperkalemia, severe acidosis, urea above 100 mg/dl, oliguria or anuria and fluid overload with pulmonary edema) was significantly higher than in patients with "pre-emptive" RRT (initiated without whatever conventional indication): adjusted odds ratio, ii.05; 95% CI, 1.03 to 4.09. Interestingly, besides patients with classic RRT but a delayed start (>12 hours from indication) showed higher crude bloodshed compared with patients with classic RRT that started early due to urgent indications (<12 hours from indication); this clan persisted later aligning for known confounders (odds ratio, 3.85; 95% CI, 1.48 to x.22). Due to the retrospective nature of this written report, it is non clear how effectively comparable the 2 populations (archetype vs pre-emptive or early vs delayed) are. The Canadian Critical Intendance Trials Group recently concluded the first pilot trial aiming to prospectively evaluate the feasibility of a protocol-driven accelerated RRT initiation39. This interesting complex trial showed how hard it would exist to carry a large multicenter prospective trial attempting to randomize two AKI populations only differing past the fourth dimension elapsed from RRT indication to treatment start. In fact, in the pilot trial, a big number of patients had to exist excluded afterward provisional eligibility per protocol pattern: those deemed by the intensivist and nephrologist in charge as requiring urgent RRT or deferral of RRT indication. This excluded cohort might unfortunately represent a sample of patients whose outcomes are potentially afflicted past pre-emptive or delayed RRT start. Even so, in the analysis of the enrolled 101 patients, the authors succeeded in their primary result. In the accelerated arm, median time to RRT offset was 7.4h. In the standard arm, 33 patients started RRT at a median of 31.6h from eligibility, and, interestingly, the other nineteen did non receive any RRT (half-dozen died and 13 recovered kidney function). Even though these preliminary results should be interpreted with caution, hard outcomes were not affected past acceleration of RRT start (mortality was 38% in the accelerated and 37% in the standard arm).
Prescription and maintenance of RRT
From a clinical standpoint, the effects of RRT dose have been systematically evaluated in the terminal ten years. After the milestone trial from the group in Vicenza back in 2000xl, CVVH dose has been indexed for the offset time to patients' body weight (mL/Kg/h), in order to highlight that this variable is of high importance in AKI patients. Two big, multicenter, randomized controlled studies published in 2009 (the randomized evaluation of normal versus augmented level (RENAL) replacement therapy report41 and in 2008, the VA/NIH Acute Renal Failure Trial Network (ATN) study42) finally clarified the concept of optimal dialysis dose. These fundamental trials were conceived to test the hypothesis concerning the impact of "intensive" RRT on difficult outcomes (namely mortality and ICU stay) when compared to "less intensive" renal back up. The RENAL study was conducted exclusively with continuous therapies (every bit this is the standard in Australia) and compared 25 mL/Kg/h CVVHDF to 40 mL/Kg/h. Using a unlike arroyo, the ATN study, conducted in North America, considered xx mL/Kg/h CVVHDF or thrice weekly intermittent dialysis equally the control group and compared information technology to 35 mL/Kg/h CVVHDF or daily IHD as the intensive arm. Apart from methodological differences, both studies confirmed that "intensive" RRT does not improve patient outcomes, and survival (although dissimilar between Commonwealth of australia'due south and U.s.' centers) was similar among compared arms. Based on the results of those trials, the accustomed dose of RRT is considered to be inside the range of 25–35 mL/Kg/h for CRRT and/or thrice weekly IHD with a Kt/V (see table on nomenclature) of 1.3.
Clearly, clinical effects of RRT dose are not limited to urea and excess body water control. Oligo anuric patients often suffer from balmy acidemia secondary to increased unmeasured anions (strong ion gap – SIG - 12.three mEq/50), hyperphosphatemia, and hyperlactatemia. This acidosis is attenuated by the alkalizing result of hypoalbuminemia. The effect on acid–base balance of IHD and CVVHDF has been evaluated43: metabolic acidosis is common in both groups and both techniques correct metabolic acidosis; yet, the rate and degree of correction may significantly differ between continuous and intermittent techniques. In the same written report43 CVVHDF was shown to normalize metabolic acidosis more speedily and more finer during the first 24 hours than IHD. IHD was also associated with a higher incidence of metabolic acidosis as compared to CVVHDF during the subsequent 2-week treatment menstruation. Appropriately, continuous RRT could be considered physiologically superior to IHD in the correction of metabolic acidosis. In a comparison between CVVH and peritoneal dialysis, all patients receiving CVVH accomplished correction of acidosis by l hours of treatment, whereas only 15% of those randomized to peritoneal dialysis achieved such correction (P < 0.001)44. Despite the results of these studies, correction of acidosis by RRT has not revealed whatsoever specific impact on outcomes.
Although safety features of CRRT machines have evolved, the possibility that CRRT may confer increased risk should not be disregarded45. In fact, as with any type of continuous extra corporeal therapy, CRRT frequently requires continuous anticoagulation therapy, which tin increase the bleeding run a risk in instance of heparin utilise or metabolic derangements in case of citrate use. Conversely, clotting of the extracorporeal circuit also occurs often with CRRT, which might contribute to blood loss and could exacerbate anemia in critically sick patients. The increased solute transfer associated with the use of CRRT might enhance removal of amino acids, vitamins, catecholamines, and other solutes. Every bit alluded to earlier, therapy downtime (the menstruation when a prescribed CRRT has not run due to unplanned interruptions) should be carefully controlled, maybe limited and eventually compensated, considering it might significantly touch dialysis commitment46–47. Following this path, it might exist speculated that the quality of care and the specific dialysis monitoring is likely to be superior when a dialysis nurse is attending the treatment session48. In society to meet the safety requirement, the new generation of CRRT machines has been implemented with a strict safe profile limiting dangerous side effects of dialytic treatments. In any example, ICU staff training is mandatory before starting the routine utilization of such monitors.
A synopsis of RRT prescription is likewise presented in Tabular array 3.
Tabular array 3. Algorithm for RRT prescription.
| Clinical variables | Operational variables | Setting |
|---|---|---|
| Fluid remainder | Net Ultrafiltration | A continuous direction of negative balance (100–300 ml/h) is preferred in hemodynamically unstable patients. |
| Adequacy and Dose | Clearance/Modality | 25–35 ml/Kg/h for CRRT, consider first CVVHDF (even if no evidence is bachelor about which modality is better). If IHD is selected, at to the lowest degree a Kt/V of 1.3 on alternate days should be targeted even if fluid residuum tin can be adequately managed only by everyday dialysis. |
| Acid–Base of operations | Solution Buffer | Bicarbonate buffered solutions are preferable to lactate buffered solutions in example of lactic acidosis and/or hepatic failure. |
| Electrolyte | Dialysate/Replacement | Consider solutions without K+ in case of severe hyperkalemia. Manage accurately MgPO4. |
| Timing | Schedule | Early and "acceptable" RRT is suggested even if no specific recommendation is bachelor. |
| Protocol | Staff/Automobile | Well-trained staff should routinely utilize RRT monitors according to predefined institutional protocols. |
Indications to finish RRT
In the specific setting of "weaning from RRT", no good evidence exists at nowadays and it is unlikely to be the case in the near future. Withal, some insights may be gleaned from contempo bachelor literature. An interesting report from the Showtime and Ending Supportive Therapy for the Kidney (BEST Kidney) investigators described electric current exercise for the discontinuation of CRRT in order to identify variables associated with successful discontinuation and whether the arroyo to discontinue CRRT therapy affected patient outcomes49. Statistical assay identified urine output and creatinine as meaning predictors of successful abeyance. The predictive value of urine output was negatively affected by the use of diuretics. Hazard factors for re-dialysis were also analyzed50: the 94 postoperative patients analyzed by these authors were considered free from RRT if after at least 30 days they did non require dialysis. Successful weaning from RRT was correlated with Sequential Organ Failure Cess (SOFA) score, age, dialysis duration and, over again, urine output. Interestingly, out of the patients who remained "RRT-complimentary" for v days later on RRT discontinuation, more than than two-thirds (20) remained RRT-gratis for upwards to 30 days.
Every bit a general recommendation, before weaning from RRT, physicians should wait for acceptable urine output (without diuretic therapy) and optimized creatinine values. Once renal function appears close to the baseline or "pre-AKI" level, it seems reasonable to interrupt the handling without any specific weaning protocol. Hereafter trials, including the identification of new biomarkers, are needed to design novel weaning protocols.
Conclusions
In recent years, slap-up technological improvements have been made in the manufacturing of extracorporeal circuits, rendering them easier to utilize, safer and more than efficient for long-term support. Modern RRT systems tin can be managed in the ICU by ane bedside nurse who is trained and experienced in excursion management, and information technology is now possible to treat patients for several weeks, or even months, without major complications. Thank you to technology development, the possibility of removing "waste products" is currently open up to several molecules, including middle-sized ones, different from creatinine. Information technology is at present becoming a reality to integrate multiple devices into a single user-friendly machine for CO2 clearance, hemoperfusion, plasma-filtration and adsorption responding to different medical needs51–58. Finally, advances in it should let the fully integrated extracorporeal claret purification arrangement to be continued to all electronic therapeutic devices, from simple syringe pumps to CRRT machines, in order to ultimately atomic number 82 to an ''artificial organ'' in a more consummate sense59. In such a detailed and diversified technological world it is of utmost importance that communication among practitioners (physicians, nurses, technicians, researchers) is homogeneous and widely accustomed. In light of this, nomenclature is a crucial aspect concerning RRT (delight see Table 4 for a list of terminology and its significance). It is extremely of import to avert a sort of "Tower of Babel" consequence by sharing a mutual languagesixty.
Table 4. Classification.
| Nomenclature | Description |
|---|---|
| Intermittent hemodialysis (IHD) | A prevalently diffusive treatment in which blood and dialysate are circulated in counter electric current manner and, more often than not, a low permeability, cellulose-based membrane is employed. Dialysate must be pyrogen gratuitous but non necessarily sterile, since dialysate-blood contact does not occur. The UF charge per unit is equal to the scheduled weight loss. This handling can exist typically performed four (to half dozen) hours thrice weekly or daily. Qb: 150–450 ml/min Qd: 300–600 ml/min. |
| Kt/V | This is an adimensional number utilized to express clearance during IHD. The numerator expresses intensity or clearance (K) per time (Kt) and denominator indicates the solute volume of distribution (5): in theory, a Kt/V of 1 implies that a dialytic session delivered with a certain Thousand of a specific solute (mostly urea) for a determined period of time (t) has completely removed the marker solute from patient volume of distribution (V). In practice, generation rate of the marker solute (and other circuitous factors) avoids blood concentration of the given solute to be zeroed. |
| Peritoneal dialysis (PD): | A predominantly deviating treatment where blood, circulating forth the capillaries of the peritoneal membrane, is exposed to dialysate. Admission is obtained past the insertion of a peritoneal catheter, which allows the abdominal instillation of dialysate. Solute and water motility is accomplished by the ways of variable concentration and tonicity gradients generated by the dialysate. This treatment can be performed continuously or intermittently. |
| Dull continuous ultrafiltration (SCUF): | Technique where claret is driven through a highly permeable filter via an extracorporeal excursion in veno-venous mode. The ultrafiltrate produced during membrane transit is non replaced and it corresponds to weight loss. It is used only for fluid control in overloaded patients (i.e. congestive eye failure resistant to diuretic therapy). Qb: 100–250 ml/min. Quf: five–xv ml/min (Figure 2). |
| Continuous veno-venous hemofiltration (CVVH): | Technique where blood is driven through a highly permeable filter via an extracorporeal circuit in veno-venous fashion. The ultrafiltrate produced during membrane transit is replaced in part or completely to reach blood purification and volume control. If replacement fluid is delivered after the filter, the technique is defined as post-dilution hemofiltration. If information technology is delivered earlier the filter, the technique is defined as pre-dilution hemofiltration. The commutation fluid can also exist delivered both pre and mail service filter. Clearance for all solutes is convective and equals UF rate. Qb: 100–250 ml/min. Quf: 15–60 ml/min (Effigy two). |
| Continuous veno-venous hemodialysis (CVVHD): | Technique where blood is driven through a low permeability dialyzer via an extracorporeal excursion in veno-venous mode and a counter current menstruum of dialysate is delivered on the dialysate compartment. The ultrafiltrate produced during membrane transit corresponds to patient's weight loss. Solute clearance is mainly diffusive and efficiency is express to small solutes only. Qb: 100–250 ml/min. Qd: 15–60 ml/min (Figure 2). |
| Continuous veno-venous hemodiafiltration (CVVHDF): | Technique where blood is driven through a highly permeable dialyzer via an extracorporeal excursion in veno-venous manner and a countercurrent flow of dialysate is delivered on the dialysate compartment. The ultrafiltrate produced during membrane transit is in backlog of the patient's desired weight loss. A replacement solution is needed to maintain fluid balance. Solute clearance is both convective and diffusive. Qb: 100–250 ml/min. Qd: fifteen–sixty ml/min. Qf: 15–60 ml/min (Figure 2). |
| Hybrid Techniques | Sustained depression-efficiency extended daily dialysis (SLEDD), prolonged daily intermittent RRT (PDIRRT), extended daily dialysis (EDD), extended daily dialysis with filtration (EDDf), extended IHD. |
| Hemoperfusion (HP): | Blood is circulated on a bed of coated charcoal powder to remove solutes by adsorption. The technique is specifically indicated in cases of poisoning or intoxication with agents that tin can exist effectively removed by charcoal. Polymixin hemoperfusion has been attempted for endotoxin removal in gram-negative septic AKI patients51. This handling may cause platelet and poly peptide depletion. |
| Plasmapheresis (PP): | A treatment that uses specific plasmafilters. Molecular weight cut-off of the membrane is much higher than that of hemofilters (100–chiliad kDa): plasma as a whole is filtered and blood is reconstituted by the infusion of plasma products such as frozen plasma or albumin. This technique is performed to remove proteins or protein-bound solutes. |
| High flux dialysis (HFD): | A handling that utilizes highly permeable membranes in conjunction with an UF control system. Due to the characteristics of the membrane, UF occurs in the proximal part of the filter that is counterbalanced by a positive pressure applied to the dialysate compartment: this causes a phenomenon called backfiltration in the distal part of the filter. Hence, improvidence and convection are combined, merely, thanks to the use of a pyrogen-free dialysate, replacement is avoided. |
| High book hemofiltration (HVHF): | HVHF is defined equally continuous loftier-volume treatment with an effluent charge per unit of 50 to 70 ml/kg/hour (for 24 hours per mean solar day) or intermittent very high-book handling with an effluent rate of 100 to 120 ml/kg/60 minutes for a 4- to 8-60 minutes flow followed by conventional renal-dose hemofiltration61. Clinical benefits of HVHF have been recently questioned. |
| High cut-off hemofiltration or Hemodialysis | A technique aimed at removing inflammatory mediators (east.thou. cytokines) in septic patients. HCO membranes are porous enough to achieve the removal of larger molecules (approximately 15 to lx kD) by diffusion. Its ability to remove cytokines in ex vivo and in vivo studies has now been shown to be greater than that of any other engineering science so far52 and has increased survival in experimental models of sepsis53. HCO therapy seems to have beneficial effects on allowed jail cell function and preliminary man studies using intermittent hemodialysis with HCO membranes take confirmed its ability to remove marker cytokines IL-six and IL-1 receptor antagonist, with a decreased dosage of norepinephrine in patients with sepsis54. Predictably, albumin losses are significant, merely may be attenuated by using HCO membranes in a diffusive rather than convective fashion while withal preserving the outcome on cytokine clearance. |
| Plasma Therapy | The term "plasma therapy" actually encompasses two therapies: plasma-adsorption and plasma exchange. In plasma-adsorption, plasma separated from claret cells flows along one or more columns that contain different adsorbents, after which the processed plasma is re-infused back to the patient. Plasma commutation is a unmarried-stride process in which blood is separated into plasma and cells and the cells are returned dorsum to the patient while the plasma is replaced with either donor plasma or albumin. With respect to sepsis, it has been argued that plasma therapy is well-nigh likely to exist effective in patients with sepsis-associated thrombotic microangiopathy55. |
| Coupled plasma filtration adsorption (CPFA) | CPFA uses a resin cartridge inserted downstream from a plasma filter, improving the removal of nonspecific septic mediators with promising results in early pocket-size trials56,57 although these have been recently doubted62. CPFA is aimed at non-selectively reducing the circulating levels and activities of both pro- and anti-inflammatory mediators during sepsis and multiorgan failure. In order to overcome the shortcomings of plasma filtration and improving the removal efficiency, CPFA uses a specific sorbent cartridge inserted in serial with, but downstream to, the plasma filter. |
| Blood purification therapies | Literature on therapeutic furnishings of claret purification therapies in septic patients is not univocal. However, a number of confounding factors brand these studies not comparable. Careful patient stratification on microbiological and clinical characteristics of sepsis together with the identification of the optimal timing for specific interventions should be the starting points for clinical application to this complex category of patients. Further data from new studies are needed to improve define the role of these advanced therapies in septic AKI-ICU patient. |
Source: https://f1000research.com/articles/5-103
0 Response to "Error 556570 Has Occurred Pleas Wait a Little While and Try Again"
Post a Comment